Headaches: A TMJ Sleep Apnea Connection?
Headaches can be more than just a common discomfort—they may be linked to underlying conditions such as TMJ disorders and sleep apnea. TMJ dysfunction can cause muscle strain and nerve irritation, leading to tension headaches, while sleep apnea disrupts oxygen flow and sleep quality, triggering morning headaches. Many individuals suffering from chronic headaches may not realize that these conditions could be the root cause. At Koala® Center For Sleep & TMJ Disorders, our experienced professionals specialize in diagnosing and treating TMJ-related and sleep apnea-induced headaches to provide lasting relief. For more information, please contact us today or request an appointment online. We have convenient locations in Bloomington IL, Peoria/Dunlap IL, El Paso TX, and Wausau WI.


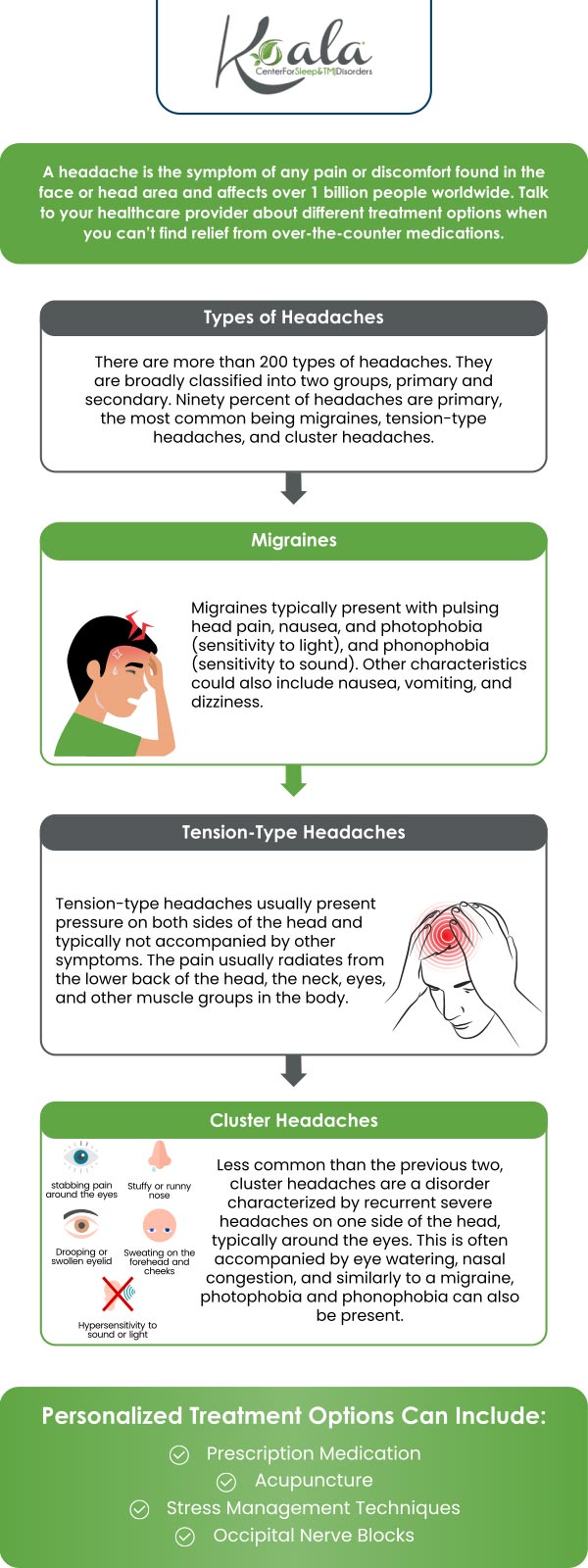
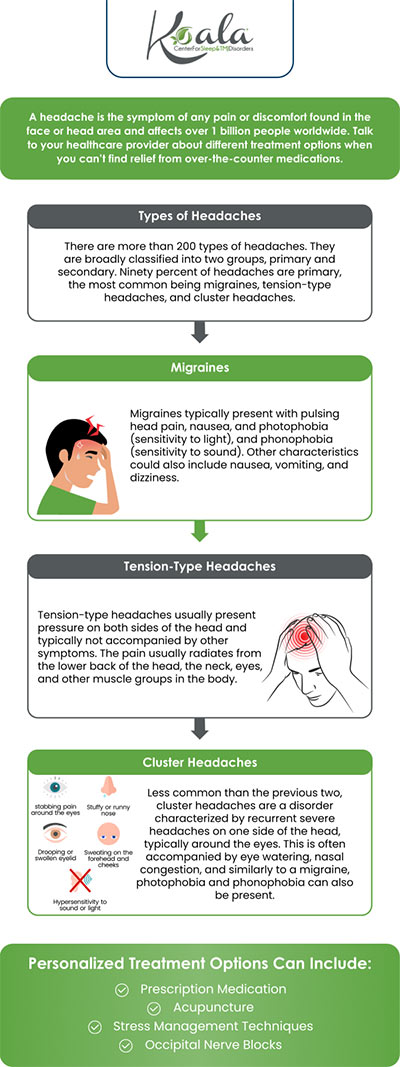
If you are one of the many people who suffer from headaches that haven’t responded to traditional treatments or medicines, if you have all but given up on trying to find the solution, you are not alone.
In today’s article, we’d like to discuss the possible causes for headaches and how they relate to sleep-disordered breathing and/or temporomandibular joint disorder.
Question: You’ve mentioned previously in your column that headaches may be an indication of sleep-disordered breathing. Can you explain the connection between the two?
Answer: It all has to do with a lack of oxygen in the bloodstream. The connection to sleep-disordered Breathing is an easy one: the airway obstruction that causes sleep disorders Breathing doesn’t let enough oxygen get to the blood. If you can’t breathe in deeply or frequently enough, you cannot get a sufficient amount of oxygen. Nor can you exhale all the carbon dioxide you’re supposed to. This is why many patients with sleep-disordered breathing wake up with headaches that may last into the afternoon. Let’s examine some common headache types. Headaches are generally classified into several basic types: sinus, cluster, tension, and migraine. You can determine which type you have by discussing it with your physician or dentist. While headaches are typically treated by your physician, improper occlusion (your bite) may play a significant role in certain types of headaches as well as other head and neck pain. One type of headache, tension headache, is by far the most common, estimated by some to be the cause of as much as 90% of all headaches. Further, there are headaches that often originate in, or pain is referred to, the muscles in your forehead.
Cluster headaches are often found in conjunction with sleep-disordered breathing and vice versa. Such headaches even accompany snoring, according to the journal Cephalgia. Patients who snore and those with obstructive sleep apnea have a high prevalence of headaches.
Scientists speculate that cluster headaches could be caused by cerebral vasodilation, a widening or opening of the blood vessels in the brain, related to an inadequate supply of oxygen in the blood (hypoxemia) or an unusually high concentration of carbon dioxide (hypercapnia) during REM (the dreaming stage) sleep.
As for your everyday, common headache, a connection exists to sleep-disordered breathing as well. In a study in Sweden, headaches were found to be more common in both men and women who snore and those who have obstructive sleep apnea than in the controls in the experiment.
Morning headaches were three times more common among male and female heavy snorers and those suffering from obstructive sleep apnea than in the general population.
Whether the headaches are of the painful vascular or cluster type and are unresponsive to medication, or they are simply an ache that seems to linger in the head from the morning to the afternoon, sleep-disordered breathing could be the reason. We recommend speaking with a health care practitioner as soon as possible to determine the cause and take care of the problem.
Question: At my last check-up, my dentist informed me that I have Temporomandibular Joint Disorder (TMJ Disorder). I snore and grind my teeth at night. Should I ask my dentist to screen me for sleep-disordered breathing?
Answer: The muscles of the temple area of the forehead are muscles that play an important part in the posturing and closing of the jaw. If your occlusion bite is not right, it can lead to abnormal tension in these muscles, one of the several possible causes of tension-type headaches, toothaches, and more bizarre symptoms. Patients with TMD have described the sensation of having something stuck in their throats when nothing is there.
It’s called “The Great Imposter.” Temporomandibular Joint Disorder (TMD) symptoms can both overlap and mimic those of sleep-disordered breathing. Many dentists consider temporomandibular joint problems to be somewhat of a gray area because the conditions associated with its complex task of permitting the movement of the jaw without friction are sometimes difficult to define and even trickier to treat.
Some dentists believe that TMD is partly the existence of a temporomandibular joint problem and partly the manifestation of a sleep-disordered breathing problem. The simplest way to understand the connection: the bruxism (teeth grinding) or jaw shifting associated with sleep-disordered breathing (occurring when sleeping patients are trying unconsciously to find the top possible positioning of their airway) may inflame the temporomandibular joint or exacerbate a problem with the joint that was pre-existing.
Headaches, clicking jaw, malocclusion (misalignment of teeth), and condyle and disc displacement are all associated with TMD. However, these symptoms often occur in patients with sleep-disordered breathing as well. Research in the journal SLEEP determined in 1993 that nocturnal headaches may be caused by temporomandibular joint disorder or triggered by “sleep disordered breathing” with very similar clinical manifestations but very different therapeutic implications.
If you have Temporomandibular Joint Disorder, we suggest you ask your dentist to screen you for Sleep Disordered Breathing. Don’t let “the Great Imposter” trick you into believing that your problem is solely a temporomandibular joint one. It may not be.
Question: If my dentist doesn’t screen for sleep-disordered breathing or temporomandibular joint disorder, where can I go?
Answer: The dentists at the Koala® Center For Sleep & TMJ Disorders are general dentists trained in neuromuscular dentistry, TMD developmental diagnosis, guided growth development, and functional appliances. “Oral appliances should be fitted by qualified dental personnel who are trained and experienced in the overall care of oral health, the temporomandibular joint, dental occlusion, and associated oral structures. “American Academy of Sleep Medicine.

Additional Services You May Need
▸ KoalaKIDZzz®
▸ Sleep Apnea
▸ Snoring
▸ TMJ Disorder
▸ Fatigue
▸ Sleep Disorders
▸ Weight Loss
▸ CPAP Alternative
▸ Oral Appliances