Oral Appliance Sleep Apnea Treatment Changed My Life
Oral Appliance Therapy (OAT) Has Proven to Be a Very Viable & Scientifically Based Treatment Option for Obstructive Sleep Apnea. For more information, please contact us today or request an appointment online. We have convenient locations in Bloomington IL, Peoria/Dunlap IL, El Paso TX, and Wausau WI.
Connie, a retired nurse, had struggled with daytime tiredness, morning headaches, irritability, and weight gain. “I had to push myself to do anything in the morning because I was always so tired,” she says.
Connie awoke one morning with chest discomfort. “My heart was racing and I checked my pulse and it was 130!” she says. Immediately I went to the emergency room,” she continues. The cardiologist said Connie needed to start Warfarin, a medication that prevents blood clots, because I was experiencing atrial fibrillation. “The blood clots could have easily traveled to my brain and caused a stroke if I hadn’t received treatment then,” says Connie.
The cardiologist also suggested Connie have a sleep study to see if a sleeping disorder could be causing her atrial fibrillation. “I had wondered in the past if my fatigue and recent morning headaches could be from sleep apnea, but didn’t realize atrial fibrillation could also arise from sleep apnea,” she continues.
According to the American Academy of Sleep Medicine, when apneas occur the amount of oxygen in the blood can drop to below 60 percent. At the same time blood pressure can soar as high as 240/130. According to the National Heart, Lung, and
Blood Institute, normal blood pressure is below 120/80. The oxygen deprivation causes the heart to pump harder to support the extra effort of the lungs trying to overcome the obstruction of the airway.
This stress triggers your body to respond in ways that may promote high blood pressure, heart disease, and other cardiovascular complications. A study in the August 1, 2010 issue of the medical journal SLEEP confirms the urgency of treating sleep apnea. Results show that people with severe, untreated sleep apnea have five times the risk of dying from a heart problem. Untreated sleep apnea can also increase your risk for depression, diabetes, gastric reflux, morning headaches, weight gain, and stroke.
Connie’s sleep study revealed that she had sleep apnea. “Both of my parents had symptoms of sleep apnea,” she says, “and looking back, I remember my dad snoring a lot. I tried to encourage them to have sleep studies, but they never did. I lost my mother from atrial fibrillation that led to a stroke,” says Connie. “I understood how dangerous untreated sleep apnea can really be and knew I needed to be treated.”
The pulmonologist recommended Connie use the oral sleep appliance to treat her sleep apnea, and recommended Dr. Rod Willey of the Illinois Institute of Dental Sleep Medicine. “I had read about the oral appliance and heard stories about people who were non-compliant to CPAP, and decided to go with the oral appliance.”
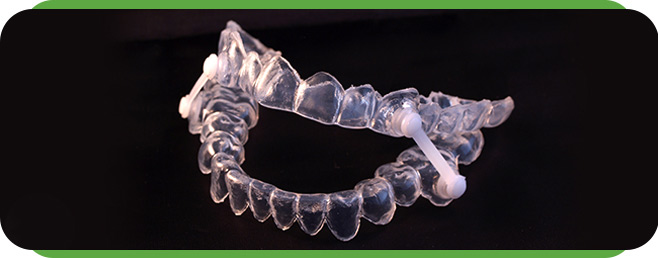
Oral Appliance Therapy (OAT) has proven to be a very viable and scientifically based treatment option for Obstructive Sleep Apnea. The American Academy of Sleep Medicine issued a statement in the 2006 issue of SLEEP that Oral Appliance Therapy was approved as the first line of treatment for those suffering from mild to moderate Obstructive Sleep Apnea, and OAT is proving to be effective for severe cases as well. The purpose of the oral appliance is to hold the jaw in a position that allows the airway to remain as open and firm as possible during sleep. Oral appliances are similar to athletic mouth guards, but less bulky and completely non-invasive.
“After treating my sleep apnea, I noticed an immediate difference in my energy levels, and it was also much easier for me to lose weight,” says Connie. “I’m not snoring and have a much better mood.” Connie can now travel without falling asleep the minute she gets into the car. She has been able to keep her atrial fibrillation under control and lowered her blood pressure.
“Treating my sleep apnea has changed my life!” she says. “So often people live with tiredness, snoring, weight gain, and discomfort because they have no idea that treating their sleep apnea can change their life!”

Additional Services You May Need
▸ KoalaKIDZzz®
▸ Sleep Apnea
▸ Snoring
▸ TMJ Disorder
▸ Fatigue
▸ Sleep Disorders
▸ Weight Loss
▸ CPAP Alternative
▸ Oral Appliances